 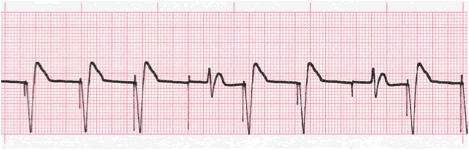
In patients with AF and slow ventricular response, only the ventricle needs to be paced, and if ventricular activity is sensed the pacing is inhibited (VVI). 
For example, patients with sinus node dysfunction but normal conduction might only need their atria paced, and if intrinsic atrial activity is sensed the pacing is inhibited (AAI). Pacemakers are classified by a sequence of 3 letters specifying 1) the chamber(s) being paced (Atrial, Ventricular, or Dual), 2) the chamber(s) being sensed (Atria, Ventricular, Dual, or none), and 3) the response to sensing (Triggered, Inhibited, Dual, or none). Atrial pacing in the right atrium produces a P wave similar to normal sinus rhythm, while right ventricular pacing mimics bundle branch block (usually LBBB, with a left axis and no R wave progression, from a pacemaker in the apex of the right ventricle). PACER mnemonic: ECG Approach to pacemaker patientsĬommon indications for permanent pacing include sinus node dysfunction causing symptomatic bradydysrhythmias, AV block, cardiac resynchronization for severe heart failure, or for termination of tachydysrhythmias. Old then new:Ĭase 9: 75 year old, history CAD, VVI pacemaker for AF, with few days weakness and presyncope. Old then new:Ĭase 3: 85 year old, DDD pacemaker for sinus pauses, with pleuritic chest pain 5 days after pacemaker insertionĬase 4: 90 year old, history CAD and CHF with biventricular pacemaker, on spironolactone, with few days of weaknessĬase 5: 75 year old, DDD pacemaker for hypertrophic cardiomyopathy, with an hour of chest pain and nauseaĬase 6: 85 year old, history inferior MI, VVI pacemaker for AF with slow ventricular response, with acute chest painĬase 7: 100 year old, history aortic stenosis and AF, VVI pacemaker for AV block, with generalized weakness, trop 300 ng/LĬase 8: 75 year old, DDD pacemaker for AV block, with weakness and confusion, HR 110 and BP 90. What’s the diagnosis, and is it related to the pacemaker or the patient?Ĭase 1: 85 year old, history of MI, DDD pacemaker for AV block, with palpitationsĬase 2: 80 year old, VVI pacer for AF with slow ventricular response, with shortness of breath, weakness and dizzy. Usually lead fracture or insulation defects.ġ.May see pacing spikes WITHIN the QRS complex.Ģ.9 pacemaker patients presented to the ED. new BBB) and cause functional UNDER-sensing. Prolonged refractory period can be 2/2 changes in the patient’s EKG complex (e.g. Failure to Sense- Pacemaker doesn’t recognize a myocardial depolarization (native activity) after it’s traveled up the lead wire.ġ.“Blanking” where the pacer doesn’t sense a normal depolarization. If patient stimulates rectus or pectoral muscle while on cardiac monitor, may see reduced pacemaker output.ģ. Can also be due to retrograde p waves, t waves, or other post-depolarization electrical activity sensing as though it was a normal potential and causing the pacemaker not to send a stimulus.ĥ.May see large P or T waves, skeletal muscle activity on EKG or may not see anything. someone painting a room, causing contraction of the pectoris). HR found b elow the lower limit set on the device and no pacemaker artifact on EKG.ġ.Pacemaker over-sensing is most common cause of failure to pace.Ģ.Lead fracture from blunt trauma due to MVA, sports, or fallsģ.Over-sensing caused by device misinterpretation of myopotentials from surrounding muscle (e.g. Failure to Pace- Pacemaker not sending a pulse to stimulate the heart. If native rate above pacemaker threshold, it naturally won’t send a signal. If myocardium is in refractory state, depolarization won’t happen.ġ.Causes include electrode displacement, wire fracture, electrolyte disturbance, medications, heart disease, MI, or exit block.Ģ.N.B. Failure to Capture- Pulse sent but myocardium doesn’t feel it. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
